Non-Surgical Root Canal Retreatment of Mandibular Incisor with Periapical Lesion
Introduction
The patient presented with a mandibular central incisor that was asymptomatic but exhibited a large periapical radiolucency on routine radiographic examination. The chief complaint was the need to address the chronic infection and prevent future acute flare-ups.
Clinical Procedure
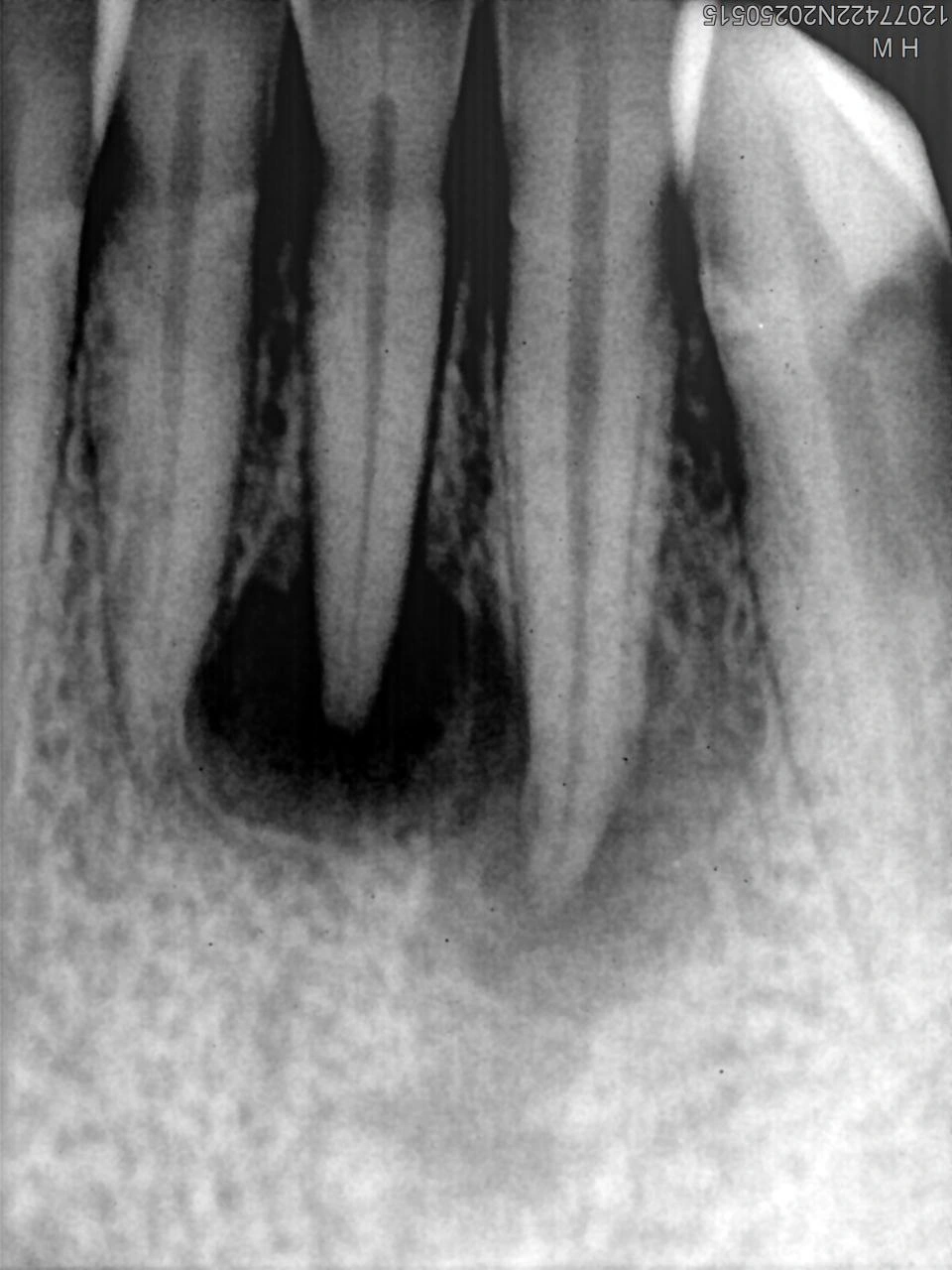
Initial Examination: preoperative findings from the radiograph (Image 1) showed a large, well-defined periapical radiolucency suggestive of chronic apical periodontitis. The tooth had an existing coronal restoration.
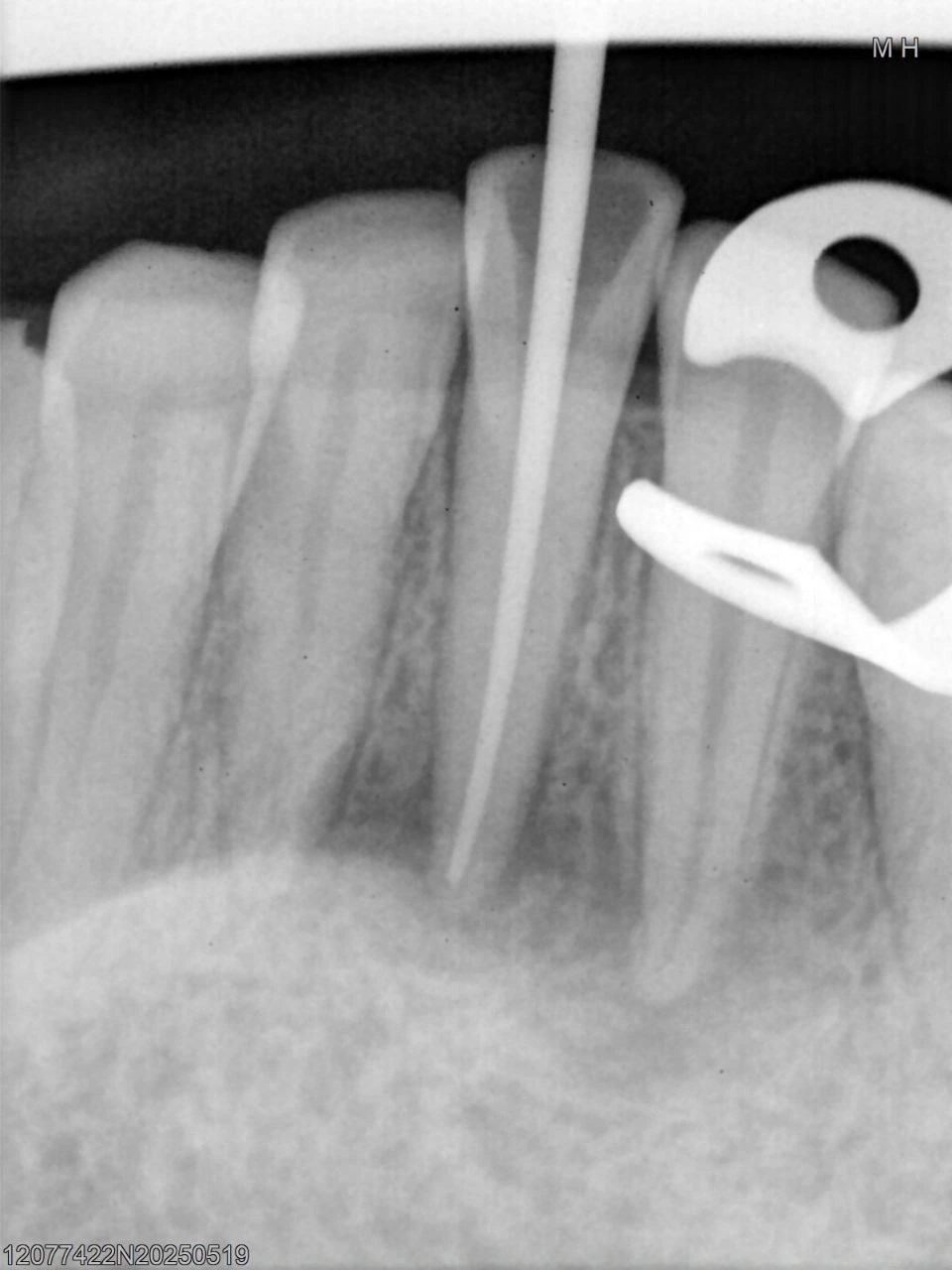
Tooth Preparation: the existing coronal restoration and access cavity were carefully removed/reopened. The canal was prepared and thoroughly irrigated with sodium hypochlorite and EDTA to clean the root canal system and eliminate bacteria. A master cone radiograph (Image 2) was taken to confirm the correct working length and tug-back of the final gutta-percha cone, ensuring the filling would extend to the radiographic apex.
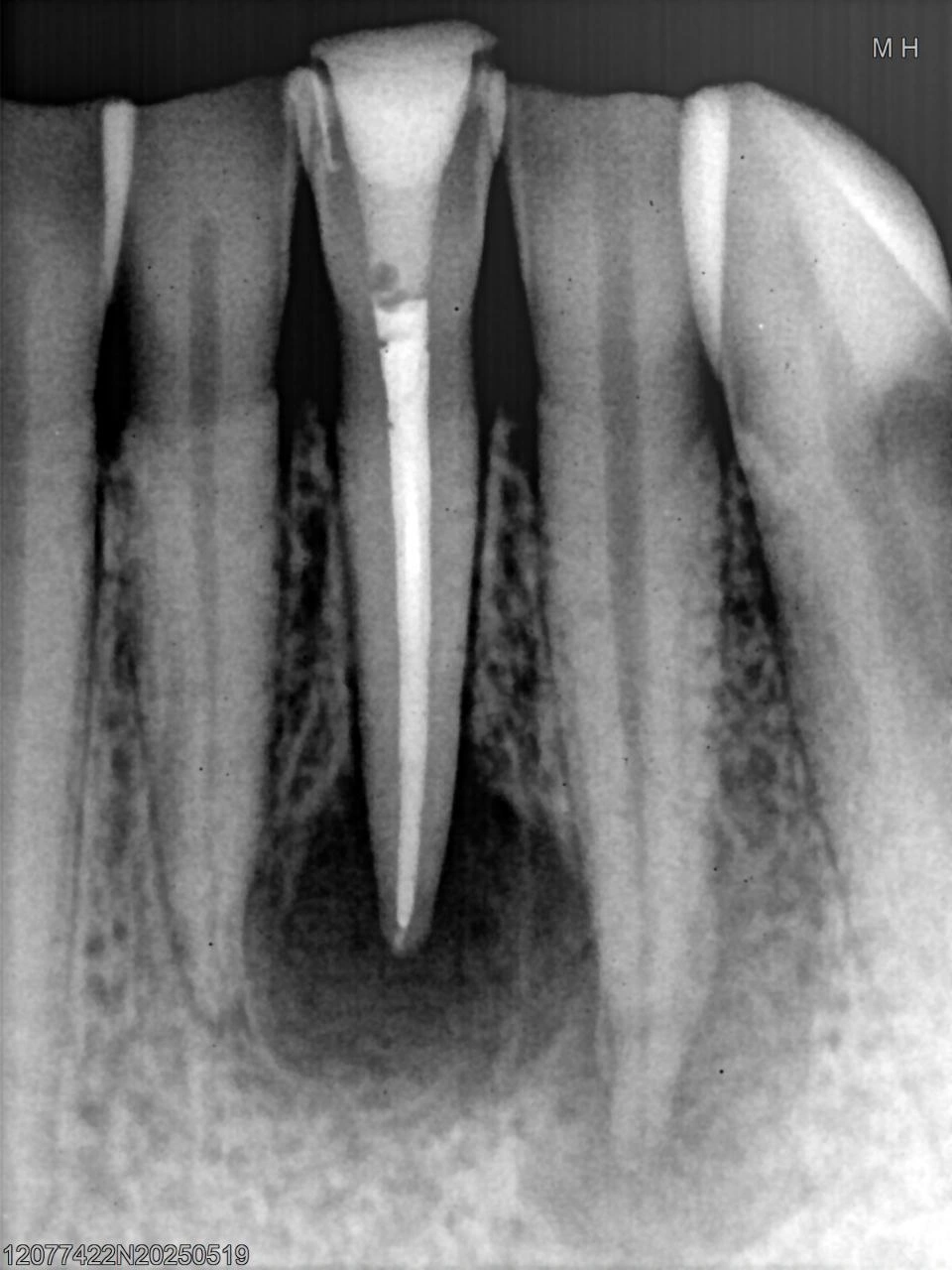
Calcium hydroxide paste: was placed as an intracanal medication for an extended period to further disinfect the canal system. Following the observation period and clinical confirmation of no symptoms, the calcium hydroxide was removed, and the root canal was three-dimensionally filled (obturated) with gutta-percha and sealer using a warm vertical condensation technique (Image 3 - Post-obturation image showing the final fill, without the master cone).
Restoration: aproper coronal seal was placed to prevent re-infection. The final coronal restoration was completed subsequently.
Outcome
The periapical lesion is expected to heal over time following the successful non-surgical retreatment and establishment of a high-quality coronal seal. The treatment was successful in resolving the source of infection, and the patient was informed of the importance of follow-up radiographs to monitor periapical bone regeneration.